Case study
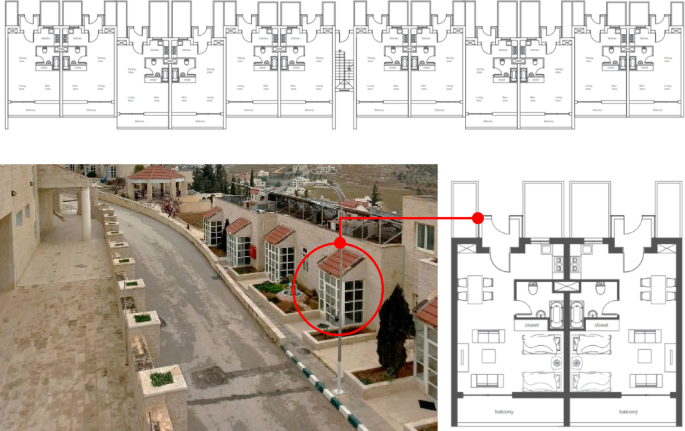
This pilot study was conducted in Darat Samir Shamma, a non-profit senior care facility located in North Amman, Jordan. The facility was selected due to its comprehensive healthcare system, including regular medical evaluations, psychiatric and social support staff, and stable residential environment conducive to environmental interventions. The facility comprises 61 apartments. Each unit is 57 m2 and contains a living room, dining area, kitchen, sleeping space, and bathroom, plus a private garden, parking space, and balcony (Fig. 1). Because all apartments share an identical layout and are insulated from external noise, they provide a controlled environment for assessing the impact of dynamic lighting on sleep.

Typical apartment layout. Floor plans redrawn by Razan Abu Hamdan; facility photograph taken by Razan Abu Hamdan.
Study sample and participant selection
A purposive sampling approach was used to recruit participants based on strict inclusion and exclusion criteria tailored to the study’s focus on sleep outcomes. Eligible individuals were aged 60 or older and physically healthy. Exclusion criteria included cognitive impairment (Montreal Cognitive Assessment (MoCA) score < 25)34, partial or complete visual impairment, and psychiatric conditions such as schizophrenia, schizoaffective disorder, or paranoia, due to their known impact on sleep regulation. To further reduce potential confounding factors, individuals cohabiting with someone diagnosed with mental illness were also excluded.
Out of 50 residents at the facility, 31 expressed interest in participating. Following screening interviews and MoCA assessments,23 were excluded: 11 for cognitive impairment, 5 for schizophrenia, 1 for schizoaffective disorder, 2 for paranoia, 2 for other mental illnesses, and 2 for visual impairment. Ultimately, eight participants (mean age = 71.5 years; range = 60–82; 3 females) met all inclusion criteria and proceeded to the experimental phase.
Although the sample size is small, this was a pilot study designed to explore feasibility and initial effects. A priori power analysis using G*Power (version 3.1) based on a Wilcoxon signed-rank test for matched pairs. Assuming large effect size (Cohen’s d ≈ 1.1), α = 0.05 (two-tailed), and a desired power of 0.80, the analysis confirmed that a minimum of eight participants would be sufficient to detect a statistically significant effect, thereby justifying the sample size for this pilot investigation.
Ethical considerations
Ethical approval (Ref: 23/161/2023; 08 June 2023) was obtained from the Institutional Review Board (IRB) at Jordan University of Science and Technology (JUST) and the administrative board of Darat Samir Shamma. Participants provided informed consent, understanding the study’s purpose, scope, and their right to withdraw at any time. All data and documents were kept confidential, adhering to Darat Samir Shamma’s privacy policies. Researchers had exclusive access to the data, ensuring compliance with ethical and institutional guidelines.
Study design
The study used a within-subject experimental design with pre- and post-test evaluations, exposing participants first to standard electric lighting and then to dynamic lighting to assess effects on sleep quality.
The independent variable was the lighting system (standard vs. dynamic light), and dependent variables included both subjective and objective sleep parameters and depressive symptoms. Objective sleep data were collected using the Withings Sleep Analyzer (WSA), a non-wearable, clinically validated device that records sleep duration, latency, efficiency, heart rate, apnea, and snoring. Subjective assessments included the Pittsburgh Sleep Quality Index (PSQI)35 and the Geriatric Depression Scale (GDS)36. A demographic form captured participant characteristics, including age, gender, education, and health status. Appendix Table 1 summarizes the measured variables, their definitions, and corresponding measurement methods. The integration of subjective and objective measures allowed for a comprehensive assessment of the lighting intervention’s impact on sleep and well-being in older adult residents.
Light intervention
The lighting intervention employed a dynamic electric lighting system designed to reflect natural day–night cycles. Light levels and correlated color temperature (CCT) were programmed to change gradually across the day: beginning with cool, bright light in the morning (500 lx, 6500 K), moderating in the afternoon, and transitioning to dim, warm light in the evening (< 100 lx, 2700 K). This profile aimed to stimulate morning alertness and promote melatonin production at night. To quantify the circadian effectiveness of the lighting, both Circadian Stimulus (CS) and Equivalent Melanopic Lux (EML) values were calculated at key time points across the day, using spectral data and vertical illuminance measurements taken at eye level (1.2 m). CS, developed by Rea, Figueiro37, estimates melatonin suppression potential based on spectral sensitivity, while EML, recommended by the International WELL Building Institute and CIE, quantifies biologically effective light aligned with ipRGC sensitivity. The lighting design targeted CS values > 0.3 during the morning and < 0.1 during the evening, with midday EML values reaching ~ 485 to account for the reduced light sensitivity in older adults27.
Light simulation
Baseline lighting measurements were collected using calibrated meters and entered into DIALux Evo 10.1, an industry-standard software compliant with CIE and IES validation protocols, to simulate and optimize fixture placement, quantity, and spectral settings in participant apartments. The simulation incorporated:
-
3D Revit modeling of apartments, considering room dimensions, window orientation, furniture layout, and daylight exposure.
-
Simulation parameters: Using the DIALux library, Philips Hue Smart LED luminaires were selected for their tunable spectrum and dimming capabilities. Simulations incorporated surface reflectance and material characteristics (e.g., curtains, wall paint, and furniture), with windows modeled at 75% transmittance based on daylight analysis. Each apartment was divided into functional zones (living, dining, and sleeping areas).
-
Optimization: The system was designed to peak at 500 lx between 8:00–12:00 p.m. decrease to < 100 lx by 8:00 p.m., and drop below 20 lx one hour before bedtime. Table 1 presents the full daily temporal lighting profile, including corresponding EML and CS values at key intervals.
-
Installation: Based on simulation outcomes (Fig. 2), existing lighting was replaced with Philips Hue LEDs in all areas except kitchens and bathrooms. The system was controlled via Philips Hue Bridge with automated scheduling of light levels and CCT adjustments throughout the day. Figure 3 shows the visual results post-installation.
Simulation results in each zone at different times of the day. Color map shows vertical illuminance (lux); blue/green = low, yellow/red = high.
Implementation was validated through post-installation measurements, confirming that target light levels were achieved at vertical eye height (1.2 m) across key zones. The lighting protocol aligned with natural daylight patterns, automatically dimming electric light when ambient light was sufficient—particularly during morning hours near windows. Continuous monitoring and periodic spot checks ensured that the programmed temporal lighting profile was maintained throughout the study. Participants had access to smart switches allowed limited brightness adjustments for personal comfort, these adjustments remained within the constraints of the automated system. No manual overrides were observed during critical measurement periods, preserving the integrity of the intervention. Self-reported activity logs were used to estimate participants’ daily light exposure in different settings. On average, participants spent 3.5 to 4 h per day in their private apartments during daylight hours, where the dynamic lighting was active. Outdoor exposure (e.g., walks or garden visits) averaged 45 min to 1 h daily. Time spent in communal indoor areas (e.g., dining or recreation rooms) ranged from 1 to 2 h daily.
Dynamic light intervention after installation in elderly apartments. All photographs taken on site by Razan Abu Hamdan.
Withings sleep analyzer
The WSA is a clinically validated, non-wearable device placed under the mattress for contact-free monitoring of sleep patterns, breathing disturbances, and cardiovascular parameters. It uses ballistocardiography (BCG) sensors and machine learning algorithms to estimate total sleep time (TST), sleep efficiency, latency, interruptions, and potential apnea events. WSA has shown good agreement with polysomnography (PSG) and actigraphy, with comparable TST and efficiency values (e.g., 392.4 ± 67.2 vs. 366.6 ± 61.2 min) and predictive accuracy of 92.6% for moderate-to-severe obstructive sleep apnea38,39,40,41. Studies also report systematic biases: WSA may overestimate sleep time and efficiency and underestimate awakenings42,43.
In this study, WSA devices were placed under participants’ mattresses to collect nightly data over 22 nights (Fig. 4). The choice of a contact-free device was guided by literature and the care facility’s recommendations, as older adults may resist or remove wearable monitors. Data were automatically synced via the Health Mate app. While WSA offered a practical and non-intrusive solution, its limitations were recognized and factored into the interpretation of outcomes.
Withings sleep analysis after fitting below participants’ mattress. Withings sleep analyzer and Withings App. All images taken and created by Razan Abu Hamdan.
The WSA recorded nightly data across all study phases for eight participants. Measured variables comprised: core sleep outcomes—sleep quality (%), total sleep time (TST), and sleep efficiency (%); timing and continuity—bedtime, out-of-bed time, time in bed (TIB), sleep-onset latency (SOL), wake after sleep onset (WASO), rise latency (RL), and interruptions (count); sleep stages—light, deep, and REM sleep (% of TST); and physiology/rest—snoring duration, heart rate, apnea index, and in-bed napping. In addition, the WSA-derived global sleep quality score integrates six indicators (duration/TST, depth, interruptions, regularity, sleep latency, and wake-up time). Full definitions and measurement units are provided in (Appendix Table 1).
The Pittsburgh sleep quality index
The PSQI is a self-report tool assessing sleep quality and disturbances through 19 questions across seven components: subjective sleep quality, habitual sleep efficiency, sleep duration, sleep latency, sleep disturbances, use of sleep medications, and daytime dysfunction. Global scores range from 0 to 21, with lower scores indicating better sleep quality (0–4: good sleep; 5–10: poor sleep; >10: severe disturbances)35. A global score above 5 typically identifies poor sleepers. The PSQI has demonstrated validity and reliability in diverse older adult populations44,45, and its Arabic version is validated for Arabic-speaking individuals46.
Aligned with adaptations used in short-term pharmacological sleep trials, participants were instructed to respond to each PSQI item based on the previous week rather than the standard one-month reference period. Prior studies have shown that this modification maintains the instrument’s reliability for short-term assessments (e.g. Figueiro, Plitnick47, Cremascoli, Sparasci48. Snyder, Cai49, and Landry, Best45.
Geriatric depression scale
The GDS is a self-reported tool developed by Yesavage and Sheikh36 to evaluate depression symptoms in older adults. The short form, used in this study, includes 15 yes/no questions36. Ten questions indicate depression with positive responses, while the remaining five do so with negative responses. Scores are categorized as 0–4 (normal), 5–8 (mild depression), 9–11 (moderate), and 12–15 (severe). The Arabic version of the GDS has demonstrated validity comparable to the English version in older adults without dementia50,51.
Study procedures
The study followed five sequential phases:
Recruitment and baseline (Days 1–12): Eligible residents were screened through interviews, cognitive assessment (MoCA). Participants followed their usual routines under standard lighting to establish a baseline.
Standard lighting (Days 13–21): Participants remained under existing electric lighting while sleep was objectively monitored using the Withings Sleep Analyzer (WSA). GDS and PSQI were recorded on Day 21.
Transition (Days 22–23): A brief transition period facilitated installation of dynamic lighting equipment while maintaining default light exposure. This brief interval ensured technical readiness without attempting full circadian resetting.
Dynamic lighting intervention (Days 24–32): Dynamic lighting system—automatically adjusting level and color temperature—was activated in apartment units. Sleep data were collected via WSA. Participants completed the GDS and PSQI at the end of this phase.
Post-intervention (Days 33–34): The original standard lighting was reinstated for a two-day washout period, matching the standard light (Days 13–21). Final GDS, PSQI, and sleep recordings were collected to evaluate sustained improvements in mood and sleep quality under standard lighting.
Controlled variables and study conditions
-
Participant activities: All participants were full-time residents who followed structured daily routines centered on meals, medical checkups, and limited social interactions. They spent most of their time indoors between 8:00 a.m. and 8:00 p.m., with only brief periods of outdoor activity or communal dining.
-
Lighting exposure: Exposure was predominantly to indoor lighting, which was automated and standardized throughout the study. Outdoor light exposure was minimal and self-reported.
-
Room environment: Apartment lighting systems were fully automated and pre-programmed to maintain consistent and controlled lighting conditions.
Statistical analysis
Objective sleep parameters from the WSA were recorded nightly for each of the eight participants across the full 22-night protocol, yielding 22 observations per participant for each of the nine measured variables. Subjective data (GDS and PSQI) were collected at the end of each of the four study phases, resulting in four time-point measurements per participant. Descriptive statistics (means, standard deviations) were reported. Given the small sample size (n = 8) and the non-normal distribution of data, paired comparisons between the standard and dynamic lighting conditions were performed using the Wilcoxon signed-rank test. Statistical significance was set at two-tailed p < 0.05, and effect sizes (r = Z/√N) were calculated. All analyses were conducted using Minitab®52.
link