Experts Sound Alarm Over Nutritional Gaps in People Taking Ozempic and Wegovy
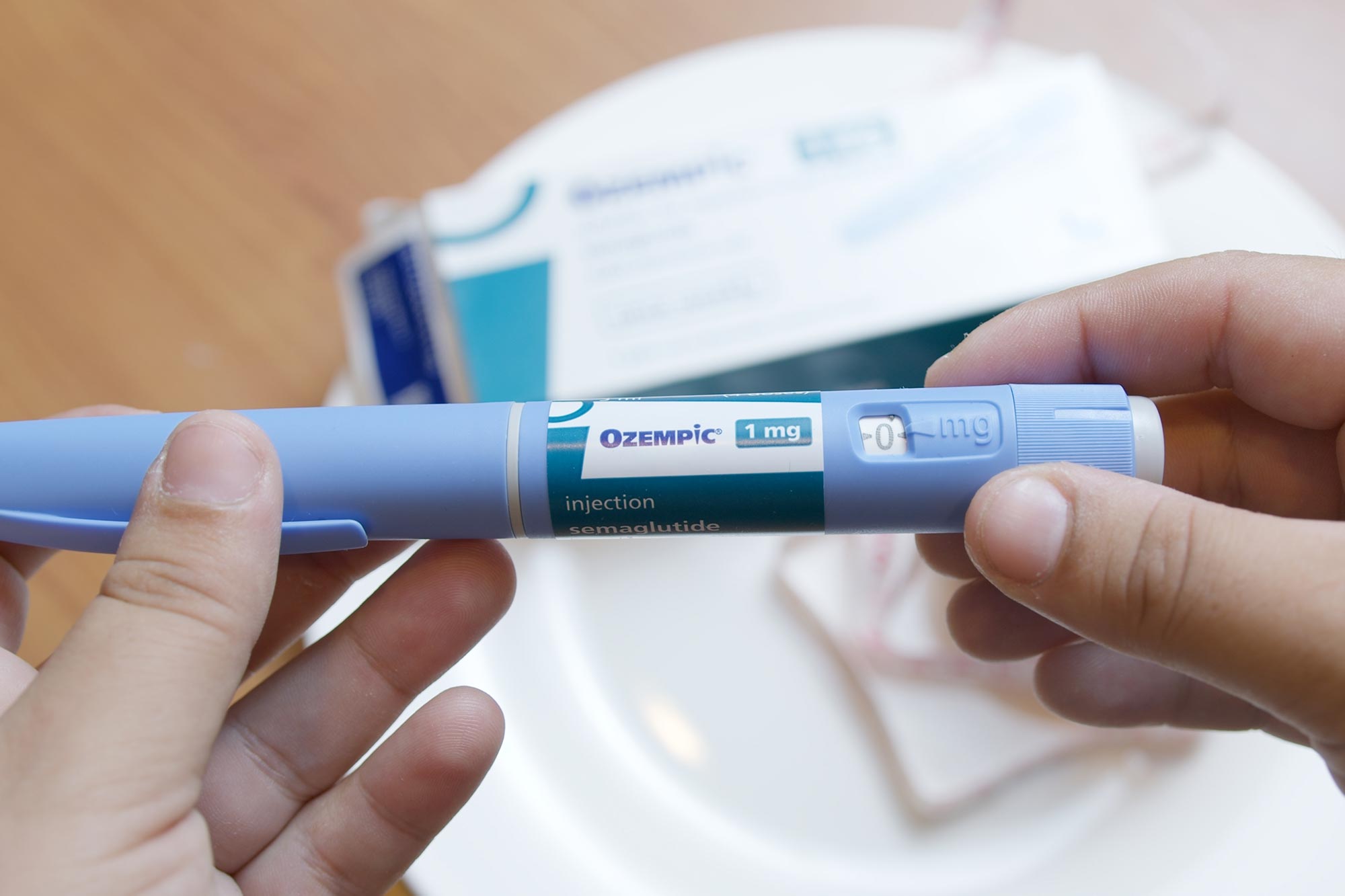
New research suggests that people using next-generation weight loss drugs may be losing weight without the nutritional support needed to protect long-term health.
People taking newer prescription weight-loss medications may not be receiving the necessary nutritional guidance to lose weight safely and maintain their health, according to researchers from UCL and the University of Cambridge. Without adequate dietary support, experts warn that people could face avoidable nutrient deficiencies and loss of muscle.
A study published in Obesity Reviews, led by Dr. Marie Spreckley of the University of Cambridge, found limited high-quality evidence on how nutritional advice is currently delivered alongside these drugs. The researchers reported major gaps in knowledge about how dietary support influences calorie intake, body composition, protein intake, and patient experiences.
Medications such as semaglutide and tirzepatide, sold under brand names including Ozempic, Wegovy, and Mounjaro, work by copying the action of glucagon like peptide-1 (GLP-1), a hormone released into the bloodstream after eating. By acting on this pathway, the drugs reduce appetite, increase feelings of fullness, and lessen food cravings.
Research shows that these treatments can lower daily calorie intake by around 16 to 39 percent, making them an effective option for people living with obesity or being overweight. Despite this, there has been little investigation into how they affect overall diet quality, protein consumption, or intake of micronutrients (vitamins and minerals). Existing evidence indicates that lean body mass, including muscle, may account for as much as 40 percent of the total weight lost during treatment.
Risks of Inadequate Nutritional Support
Dr. Adrian Brown, an NIHR Advanced Fellow from the Centre of Obesity Research at UCL, the study’s corresponding author, said: “Obesity management medications work by suppressing appetite, increasing feelings of fullness, and altering eating behaviors, which often leads people to eat significantly less. This can be highly beneficial for individuals living with obesity, as it supports substantial weight loss and improves health outcomes.
“However, without appropriate nutritional guidance and support from healthcare professionals, there is a real risk that reduced food intake could compromise dietary quality, meaning people may not get enough protein, fibre, vitamins, and minerals essential for maintaining overall health.”
Access to Treatment and Gaps in Care
Guidance from the National Institute for Health and Care Excellence (NICE) recommends semaglutide as a weight management option for people who meet specific criteria, including a body mass index (BMI) of at least 35.0 kg/m2 and comorbidity (that is, they also have other conditions such as type 2 diabetes, cardiovascular disease, etc). The guidance also makes clear that when prescribed through the NHS, the medication should be used as part of a wider program that includes a reduced-calorie diet and increased physical activity in adults.
In reality, most people obtain these drugs through private providers. Around 1.5 million people in the UK are currently using GLP-1 medications, and an estimated 95 percent access them privately. In these settings, patients do not always receive consistent nutritional advice or ongoing dietary support.
Dr. Marie Spreckley, from the Medical Research Council (MRC) Epidemiology Unit at the University of Cambridge, said: “Use of GLP-1 receptor agonist therapies has increased rapidly in a very short period of time, but the nutritional support available to people using these medications has not kept pace. Many people receive little or no structured guidance on diet quality, protein intake, or micronutrient adequacy while experiencing marked appetite suppression.
“If nutritional care is not integrated alongside treatment, there’s a risk of replacing one set of health problems with another, through preventable nutritional deficiencies and largely avoidable loss of muscle mass. This represents a missed opportunity to support long-term health alongside weight loss.”
Poor intake of essential micronutrients can increase the risk of symptoms such as fatigue, weakened immune function, hair loss, and osteoporosis. At the same time, reductions in lean mass, most commonly muscle, can raise the likelihood of weakness, injury, and falls.
Limited Evidence and Lessons From Bariatric Surgery
The researchers identified just 12 studies that looked at nutrition and diet alongside treatment with semaglutide or tirzepatide. Even then, as the trials varied widely in their approaches to dietary advice and nutritional assessment and lacked standardized protocols and reporting, it was difficult to reach robust conclusions to inform the optimal support for people taking weight loss drugs.
Given the widespread – and increasing – use of these medications and the urgency of providing advice to individuals using the drugs, as well as calling for more research, the researchers argue that we can turn to what has been learnt from the guidance and support offered alongside weight loss surgery, such as gastric bands, which leads to similar outcomes to GLP-1 drugs.
Dr. Cara Ruggiero, co-author from the MRC Epidemiology Unit at the University of Cambridge, said: “While GLP-1 receptor agonists are increasingly used, there remains a clear gap in structured nutritional guidance. In the interim, we can draw on well-established post-bariatric nutrition principles. Our previous work highlights the importance of prioritizing nutrient-dense foods including high-quality protein intake, ideally distributed evenly across meals, to help preserve lean mass during periods of reduced appetite and rapid weight loss.”
Diet Quality, Fat Intake, and Eating Patterns
While there was insufficient evidence from the studies to recommend strict low-fat diets to complement the weight loss drugs, some observational studies found that people on the treatments often consumed excessive levels of total and saturated fat. This suggests that there might be a need for individualized fat intake guidance, aligned with broad national recommendations, the team says.
Similarly, although meal frequency was not explicitly tested in most trials, they say that strategies such as small, frequent meals may help reduce common side effects such as nausea and improve tolerability, especially in the early stages of treatment.
In calling for more research in this area, the team says it is important that people who use the treatments are consulted to help identify the types of information and wrap-around support that are most meaningful and needed in real-world care. They have launched AMPLIFY (Amplifying Meaningful Perspectives and Lived experiences of Incretin therapy use From diverse communitY voices) to understand how people experience next-generation weight loss therapies when used for weight management.
Dr. Spreckley, who is leading AMPLIFY, said: “These medications are transforming obesity care, but we know very little about how they shape people’s daily lives, including changes in appetite, eating patterns, wellbeing, and quality of life. That’s what we’ll explore, working in particular with people from communities historically under-represented in obesity research, to help shape the future of obesity treatment.”
Reference: “Nutrition Strategies for Next-Generation Incretin Therapies: A Systematic Scoping Review of the Current Evidence” by Marie Spreckley, Cara F. Ruggiero and Adrian Brown, 7 January 2026, Obesity Reviews.
DOI: 10.1111/obr.70079
The research was funded by the National Institute for Health and Care Research (NIHR), with additional support from the Medical Research Council and the NIHR UCLH Biomedical Research Centre.
Never miss a breakthrough: Join the SciTechDaily newsletter.
Follow us on Google and Google News.
link